Managing dental pain in pets is crucial for their health and well-being. Proper pain control not only ensures comfort during procedures but also prevents long-term issues like anxiety and health complications. Here’s what you need to know:
- Why It Matters: Dental pain can cause serious health problems, including infections that spread to the heart, kidneys, and liver.
- Common Causes: Periodontal disease, fractured teeth, and conditions like tooth resorption are leading sources of pain.
- Signs of Pain: Look for changes like avoiding food, drooling, bad breath, or behavioral shifts like pawing at the face.
- Pain Management Steps:
- Pre-procedure: Medications like opioids, NSAIDs, and nerve blocks reduce pain before it starts.
- During procedure: Anesthesia and constant monitoring ensure safety and comfort.
- Post-procedure: Medications like NSAIDs and opioids, along with cold therapy and quiet recovery spaces, aid healing.
- Prevention: Daily brushing, dental chews, and regular vet exams can help prevent painful dental issues.
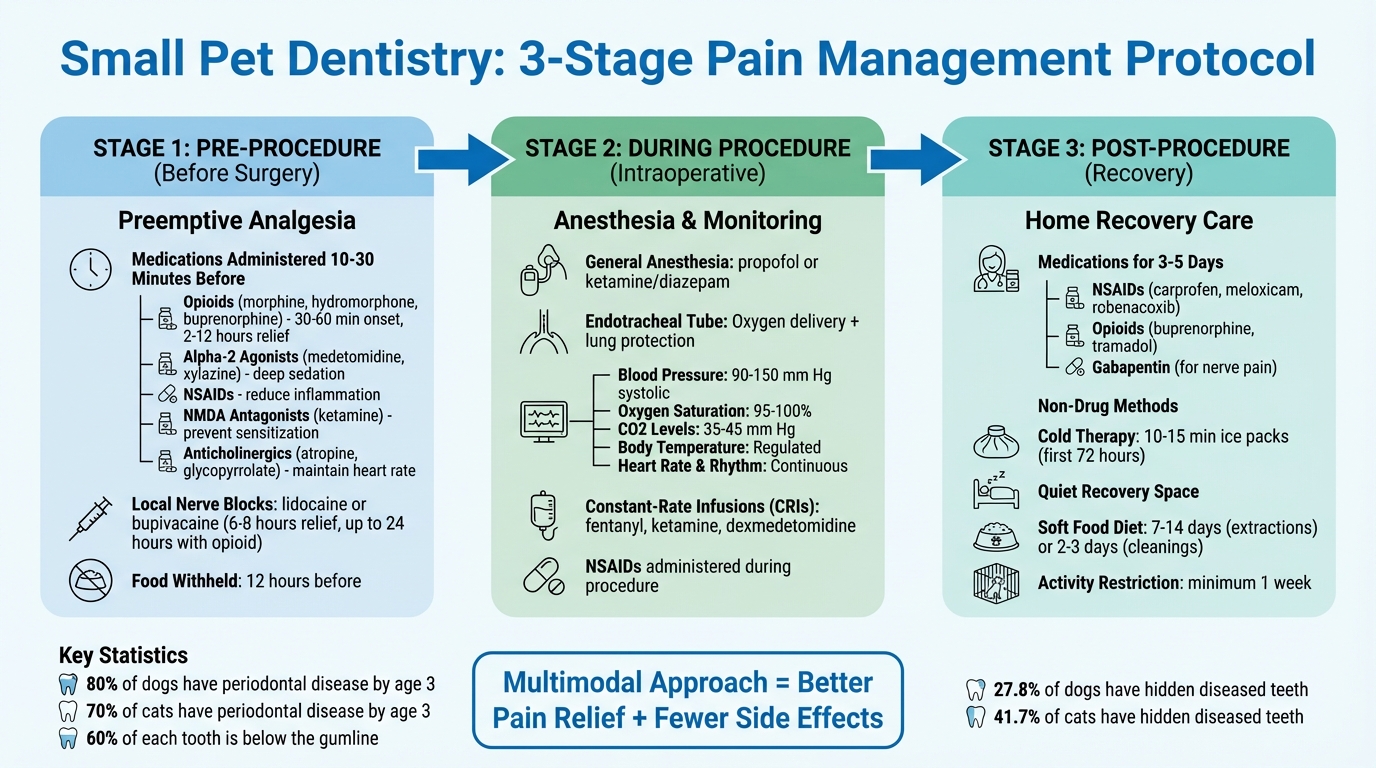
Three-Stage Pain Management Protocol for Pet Dental Procedures
Episode 166 – Inside Veterinary Dental Tech: Pain Control, Charting & Radiograph Efficiency
sbb-itb-e212914
How Dental Pain Affects Small Pets
Dental issues in small pets can do more than just cause discomfort – they can alter behavior and seriously impact overall health. Knowing the causes and signs of dental pain is essential for timely intervention, potentially preventing minor issues from escalating into major health problems.
What Causes Dental Pain
The most common cause of dental pain in pets is periodontal disease, a condition that affects over 80% of dogs and 70% of cats by the age of three. It starts with plaque forming on teeth shortly after eating. Without regular brushing, this plaque hardens into tartar (calculus) within 48 hours. Tartar creates a safe haven for bacteria, which can invade below the gumline. The resulting immune response damages the surrounding bone and tissue, leading to pain and infection.
Another frequent cause of dental pain is fractured teeth, often from chewing on hard objects like bones, antlers, or hooves. A cracked tooth can expose the sensitive pulp and nerve, potentially resulting in chronic infections or painful abscesses. Cats are particularly prone to tooth resorption, a condition where the tooth structure dissolves from within, causing significant discomfort.
Other painful dental conditions include stomatitis (inflammation and ulceration of the mouth), malocclusions (misaligned teeth that injure soft tissues), oral tumors, cysts, and abscesses. Alarmingly, more than half of each tooth lies hidden below the gumline, meaning serious disease and pain can develop without visible symptoms.
Signs Your Pet Has Dental Pain
Pets are experts at hiding pain, often masking even severe dental issues. Instead of crying out, they may show subtle changes in behavior. Watch for signs like dropping food, chewing on one side of the mouth, suddenly preferring soft food over kibble, or avoiding the food bowl completely.
Physical symptoms can include excessive drooling (sometimes tinged with blood), bad breath, jaw trembling, mouth chattering, and facial swelling. Behavioral clues might involve pawing at the mouth, rubbing the face on furniture, or avoiding head pats. Cats may stop grooming, leading to a scruffy, matted coat. Dr. Louise Murray from the ASPCA Animal Hospital highlights the severity of dental pain:
Pets with dental disease are often in severe pain – imagine having not just one toothache, but many.
The effects of untreated dental pain can spread far beyond the mouth. Bacteria from infected teeth can enter the bloodstream, causing chronic inflammation that harms the heart, kidneys, and liver. In advanced cases, jaw fractures can occur due to bone loss, and abscesses can create draining tracts in the face. Many owners mistake reduced activity or irritability for signs of aging, when in fact, chronic dental pain is the culprit. After dental treatment, owners often notice a dramatic transformation, describing their pet as happier and more energetic.
Recognizing these causes and symptoms is the first step toward managing dental pain effectively, even before treatment begins.
Managing Pain Before Dental Procedures
Pain management for pets starts well before the actual dental procedure. Veterinarians often use a method called preemptive analgesia to block pain signals before they reach the central nervous system. This approach not only ensures your pet’s comfort but also reduces the amount of general anesthesia needed, making the procedure safer. Additionally, it helps prevent a phenomenon known as the "wind-up" effect, where the spinal cord becomes overly sensitive to pain, making it harder to manage discomfort later.
Pre-Procedure Medications
Before anesthesia begins, your veterinarian will likely administer a combination of medications to prepare your pet. These are typically given 10 to 30 minutes in advance and may include:
- Opioids like morphine, hydromorphone, or buprenorphine, which are key to managing pain. Buprenorphine, for example, takes 30 minutes to an hour to take effect, and its relief can last anywhere from 2 to 12 hours depending on the dose.
- Alpha-2 agonists such as medetomidine or xylazine, which provide deep sedation and muscle relaxation. These work well with opioids, allowing for lower doses of each medication while achieving better results.
- NSAIDs (non-steroidal anti-inflammatory drugs) may be used in pets with normal circulation to reduce inflammation and pain.
- NMDA antagonists like ketamine, which help prevent central sensitization.
- Anticholinergics such as atropine or glycopyrrolate, which maintain heart rate and reduce excessive drooling during the procedure.
For pets prone to anxiety, oral medications like gabapentin or trazodone may be given before the visit to help keep them calm and enhance the overall pain management plan. Additionally, it’s important to withhold food for 12 hours before anesthesia to reduce the risk of aspiration, though water is typically allowed until the morning of the procedure.
To complement these medications, veterinarians often use local nerve blocks to target pain more directly.
Local Nerve Blocks
Local nerve blocks are a powerful tool for managing pain during dental procedures. These injections deliver anesthetics like lidocaine or bupivacaine directly to nerves in the mouth, numbing specific areas completely. Dr. Brett Beckman, a board-certified veterinary dentist, highlights their importance:
Nerve blocks not only provide excellent postoperative analgesia but also contribute extensively to maximizing the safety of the anesthetic event.
These blocks work by preventing pain signals from traveling along nerve pathways through sodium channel blockade. As Dr. Michael Peak, DVM, DAVDC, explains:
If we block the stimulus before it starts, then theoretically, pain management should be much easier.
By using nerve blocks, pets can remain under lighter general anesthesia, which helps keep blood pressure, heart rate, and breathing more stable throughout the procedure. Bupivacaine, for instance, typically provides 6 to 8 hours of pain relief, and when paired with an opioid like buprenorphine, this relief can extend up to 24 hours.
Veterinarians commonly use blocks such as:
- Infraorbital for the upper front teeth.
- Caudal maxillary for the entire upper jaw on one side.
- Middle mental for the lower front teeth.
- Caudal mandibular for all lower teeth on one side.
To ensure safety, veterinarians always aspirate the syringe before injecting to confirm the needle isn’t in a blood vessel. When done correctly, using proper doses – usually 1 to 2 mg/kg – nerve blocks are both effective and safe.
These combined strategies set the stage for safer and more effective dental procedures. Next, we’ll look at how pain is managed during the dental work itself.
Pain Control During Dental Work
During anesthesia, the veterinary team prioritizes effective pain control to ensure your pet’s safety and comfort throughout the procedure. This involves carefully balancing anesthetic drugs, closely monitoring vital signs, and using pain medications. Here’s a closer look at how anesthesia and pain management work together during dental treatments.
Anesthesia and Patient Monitoring
General anesthesia is crucial for dental procedures because it ensures your pet stays still, allowing safe and thorough access to their mouth. To induce anesthesia, veterinarians often use drugs like propofol or a combination of ketamine and diazepam, which help your pet transition smoothly into unconsciousness. Once anesthetized, an endotracheal tube is placed to deliver oxygen and anesthetic gas while also protecting the lungs from water and debris during the cleaning process.
Throughout the procedure, a dedicated team member monitors five critical parameters:
- Blood pressure: Maintained between 90 and 150 mm Hg systolic
- Oxygen saturation: Kept between 95% and 100%
- Carbon dioxide levels: Held steady at 35 to 45 mm Hg
- Body temperature: Closely regulated
- Heart rate and rhythm: Continuously tracked
Dr. Jan Bellows, DVM, DAVDC, DABVP, FAVD, emphasizes the importance of capnography in monitoring ventilation:
"End-tidal carbon dioxide (ETCO2) monitoring through capnography often is called the ‘anesthesia disaster early-warning system.’ Vitally important, it is the only parameter that thoroughly reflects a patient’s ventilatory status, and it can signal problems within two breaths".
An intravenous catheter is kept in place during the procedure to provide fluids that support blood pressure and to allow immediate access for emergency medications if needed. Anesthetic depth is carefully adjusted based on clinical indicators like jaw tone and blink reflex.
Pain Relief Medications During Treatment
Precise pain management during dental work is guided by constant monitoring of your pet’s vital signs. Veterinarians use a multimodal approach, combining different pain medications to target various points in the pain pathway, which is far more effective than relying on a single drug.
Constant-rate infusions (CRIs) are commonly used to deliver medications like fentanyl, ketamine, or dexmedetomidine steadily throughout the procedure. These infusions not only provide consistent pain relief but also reduce the amount of inhaled anesthetic gas required, improving overall safety. Ketamine is particularly effective at preventing "wind-up" pain, a condition where the spinal cord becomes overly sensitive to pain signals.
Pre-administered nerve blocks keep specific areas numb, allowing for lighter anesthesia levels while ensuring your pet stays comfortable. For pets with conditions like kidney disease, specialized protocols – such as maintaining a mean arterial pressure between 70 and 80 mm Hg – are used to safeguard organ function.
To further manage pain and inflammation, NSAIDs like robenacoxib or meloxicam are often administered during the procedure. These medications help ease discomfort as your pet begins to wake up, ensuring a smooth transition from intraoperative to postoperative pain relief. This comprehensive approach ensures your pet’s comfort throughout the entire process.
Pain Relief After Dental Procedures
Once your pet wakes up from anesthesia, the next step is managing their pain at home during recovery. Your veterinarian will typically prescribe medications for 3–5 days after the procedure to ensure your pet stays comfortable. The key to effective pain relief is to address discomfort proactively, rather than waiting for visible signs of pain. Below, we explore both medication-based and non-drug strategies to help your pet recover comfortably.
Medications for Recovery Pain
Many veterinarians use a combination of medications to address pain from different angles, a method known as multimodal analgesia. Dr. Sandra Allweiler, DVM, DACVAA, explains:
Multimodal analgesia combines drugs to enhance pain relief and reduce side effects.
NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) are often the first line of defense for post-dental pain. Medications like carprofen, meloxicam, or robenacoxib help reduce inflammation and swelling at the surgical site by blocking enzymes that produce prostaglandins. For cats, robenacoxib can be used for up to three days, while meloxicam is limited to a single dose in the U.S.. Keep an eye out for warning signs such as behavior changes, reduced appetite, skin redness, scabs, tarry stools, or vomiting (known as the "BEST" signs). If any of these occur, contact your veterinarian immediately.
For more invasive procedures, opioids are often prescribed. Buprenorphine is a popular choice due to its strong pain relief and minimal side effects. Cats may receive Simbadol, which provides 24-hour relief with just one subcutaneous injection. Tramadol is another option, though cats metabolize it more effectively than dogs, with a bioavailability of 93% in cats compared to 65% in dogs.
If nerve pain or central sensitization is a concern, gabapentin may be prescribed to block pain signals by modulating calcium channels. Some veterinarians may also use amantadine, which prevents chronic pain by targeting NMDA receptors.
It’s crucial to stick to the prescribed medication schedule, as pets often hide their pain. If your pet has been on strong pain medication for several days, your veterinarian may gradually reduce the dosage to prevent rebound pain.
Other Pain Relief Methods
In addition to medications, there are several non-drug options to make recovery more comfortable for your pet.
Cold therapy can be a simple yet effective way to reduce swelling and numb the surgical area during the first 72 hours after surgery. Wrap an ice pack in a towel and apply it to the outside of your pet’s face for 10–15 minutes at a time. This can reduce swelling up to 1 inch deep.
Creating a calm, quiet recovery space is another way to ease stress. Cats may prefer hiding spots under beds or behind furniture, while dogs might feel more secure in a crate with soft bedding. Keeping food, water, and litter boxes close by minimizes unnecessary movement and effort.
Some veterinary practices also offer acupuncture as a complementary treatment. Dr. Sandra Allweiler highlights its benefits:
Acupuncture is a safe, well-tolerated treatment and is shown to decrease pain from inflammation, neuropathy, and cancer, as well as visceral pain.
This technique works by triggering the release of natural opioids and activating the body’s pain-blocking pathways.
If your pet received a mandibular nerve block during the procedure, be vigilant during the first few hours of recovery. Pets may accidentally chew on their numb tongue or lips, so positioning them in sternal recumbency (lying on their chest) can help prevent this.
These strategies, combined with attentive care, can make a big difference in your pet’s recovery process.
Home Care During Recovery
Setting Up a Comfortable Recovery Space
For the first 48–72 hours after your pet’s dental surgery, set up a quiet recovery area to help them rest and heal. Choose a low-traffic spot where they won’t be disturbed. Since pets can struggle to regulate their body temperature after anesthesia, keep the area at a moderate, comfortable temperature. Provide soft bedding to support them while they’re groggy.
Make sure the space is free of hazards like stairs or high furniture – disorientation from anesthesia can increase the risk of falls. Dim the lighting to create a soothing environment, and place food and water close by to limit unnecessary movement. Offer small, frequent meals (around 3 to 4 times daily) to reduce the chances of nausea or vomiting. If your pet had extractions, stick to a soft food diet for 7 to 14 days. For simple cleanings, 2 to 3 days of soft food is usually enough.
During the first 12–24 hours, keep a close eye on your pet. Restrict their activity and, for dogs, use a leash during outdoor breaks. Avoid letting them jump, climb, or engage in rough play for at least a week. Check the surgical site once or twice daily for redness, swelling, or discharge – these could be signs of infection. This safe, calm setup will help your pet recover smoothly, but it’s equally important to watch for warning signs that might require veterinary attention.
Warning Signs That Need Veterinary Care
Even with a proper recovery setup, you’ll need to monitor your pet for symptoms that could signal a problem. While mild discomfort and drowsiness are normal, certain signs should prompt a call to your veterinarian. The American College of Veterinary Surgeons emphasizes:
Pain and its effects can slow recovery and prolong illness if it is not treated appropriately.
Pay close attention to your pet’s eating habits. If a cat refuses to eat for more than 24 hours or a dog for more than 48 hours, it’s time to call the vet. Cats are especially vulnerable to hepatic lipidosis if they stop eating entirely. Blood-tinged saliva is normal for the first 24–48 hours, but active dripping, pooling blood, or large clots in the mouth require immediate attention.
Breathing issues are another red flag. If your pet is struggling to breathe, panting excessively, or gasping, contact your vet right away. Check their gum color periodically by lifting their lip – healthy gums should be pink and moist. Pale, white, blue, or dry and sticky gums could indicate poor circulation or oxygen levels and need urgent care.
| Symptom Category | Normal Recovery Signs | Warning Signs (Contact Vet) |
|---|---|---|
| Activity Level | Sleepy/groggy for 12–24 hours | Collapse, seizures, or inability to stand |
| Oral Discharge | Pinkish, blood-tinged saliva | Active dripping blood, pus, or foul odor |
| Appetite | Hesitant to eat during the first 12 hours | Refusal to eat >24h (cats) or >48h (dogs) |
| Breathing | Occasional slight cough (from tube) | Difficulty breathing or excessive panting |
| Gum Color | Pink and moist | Pale, white, blue, or dry/sticky |
| Behavior | Quiet and resting | Aggression, constant whining, or hiding |
Be alert for signs of breakthrough pain, such as whining, restlessness, hiding, a hunched posture, or pawing at the face. These behaviors may mean the prescribed pain medication isn’t working well enough. If your pet experiences persistent vomiting or diarrhea, especially after taking anti-inflammatory medications, stop the medication and contact your vet immediately.
Preventing Dental Pain Long-Term
Daily Dental Care at Home
Brushing your pet’s teeth daily is one of the most effective ways to prevent plaque buildup and reduce the risk of periodontal disease. Use a toothpaste specifically made for pets – flavors like poultry or beef work well – and pair it with a soft-bristled toothbrush for the best results.
If your pet isn’t a fan of brushing right away, don’t worry. Start slowly by getting them used to having their teeth touched. Let them lick a small amount of pet toothpaste as a treat, then transition to using a finger brush or toothbrush. Hold the brush at a 45-degree angle and use small circular motions to clean their teeth. Aim for daily brushing, but even three times a week can make a difference. Introducing this habit early – between 10 weeks and 10 months – can help pets accept the routine more easily.
For added protection, consider using other dental care products. Items with the Veterinary Oral Health Council (VOHC) seal are scientifically proven to reduce plaque or tartar by at least 20%. Options include dental chews like Greenies or C.E.T. VeggieDent, water additives such as Vetradent or TropiClean, and dental diets like Hill’s Prescription Diet t/d. Be cautious with hard chews or toys, as they can lead to tooth fractures.
While daily care is key, it works best when combined with regular professional dental exams.
Regular Veterinary Dental Exams
Home care is important, but professional veterinary exams are essential for spotting issues you might miss. Even with consistent brushing, regular dental checkups help catch hidden problems early. Most veterinarians recommend dental evaluations every six to twelve months, with smaller intervals for senior pets or breeds prone to dental issues.
Small breeds and flat-faced pets need extra attention due to their higher risk of dental problems. Professional cleanings under anesthesia are typically advised every 1–2 years, though smaller dogs and cats may require them more frequently. These exams are especially important because pets often hide dental pain. X-rays have shown that 27.8% of dogs and 41.7% of cats had diseased teeth that seemed normal during visual inspections.
Conclusion
Effective pain management is a cornerstone of your pet’s health and recovery, especially when it comes to dental care. Dental pain can trigger stress hormones, which can slow healing, increase the risk of infection, and hinder nutrient absorption. Considering that around 60% of each tooth is hidden below the gumline and most pets show signs of dental disease by the age of 3, addressing pain at every stage of treatment is essential.
Using a multimodal approach – such as preemptive medications, local nerve blocks, and thorough post-operative care – can block pain signals at multiple points in the nervous system. Collaborating with your veterinarian is key to creating a care plan tailored to your pet’s needs. Pre-anesthetic testing ensures the safest drug protocol, while advanced diagnostics like X-rays uncover hidden pain sources that might not be apparent during a routine exam. Emily Singler, VMD, AAHA‘s Veterinary Content Specialist, underscores the importance of dental health:
The small risk posed by the use of general anesthesia is greatly outweighed by the benefits of maintaining or improving your pet’s dental health, since advanced dental disease can lead to serious problems not only in the mouth but in other parts of the body like the heart and the kidneys.
FAQs
How can I tell if my pet is hiding dental pain?
Pets are experts at masking dental pain – it’s a survival instinct that makes spotting problems tricky until they escalate. Keep an eye out for warning signs like excessive drooling (sometimes tinged with blood), pawing at their face, trembling jaws, or unusual mouth movements like chattering. Changes in eating habits, such as dropping food or suddenly favoring softer options, can also signal discomfort.
Behavioral shifts are another red flag. If your pet seems more irritable, sleeps more than usual, or avoids having their face touched, it might be time to investigate. Catching these signs early can make a big difference in preventing more serious complications down the road.
What questions should I ask my vet about anesthesia and monitoring?
When discussing anesthesia for your pet, it’s important to cover all the bases. Ask your vet about pre-anesthesia lab work – this can help identify any underlying health issues that might affect the procedure. Additionally, find out how they monitor key metrics during anesthesia, such as:
- Blood pressure
- Oxygen saturation
- End-tidal CO2
- ECG
- Respiratory rate
- Body temperature
These measurements are crucial for ensuring your pet stays stable and safe during the procedure. You should also ask about their safety protocols and how they handle potential risks associated with anesthesia. Understanding their approach can give you peace of mind about your pet’s well-being throughout the process.
How do I know if my pet’s pain meds are causing side effects?
Watch for any shifts in your pet’s behavior or physical health. Signs like vomiting, diarrhea, loss of appetite, lethargy, or unusual aggression could indicate an issue. More serious symptoms, such as yellowing gums, changes in urination, or reluctance to move, require urgent attention. Reach out to your veterinarian right away if you notice these warning signs. Routine vet visits are essential to confirm that the medication is working safely and effectively to manage your pet’s pain.










