Chronic respiratory conditions in small pets, like feline asthma, chronic bronchitis, or tracheal collapse, develop gradually and can severely impact breathing. Early detection and consistent care are key to improving your pet’s quality of life. Watch for subtle signs such as sneezing, wheezing, nasal discharge, lethargy, or changes in posture. Small pets are particularly vulnerable due to their size, rapid metabolism, and sensitivity to irritants like smoke, dust, or ammonia from bedding.
Key management strategies include:
- Veterinary care: Medications like corticosteroids and bronchodilators reduce inflammation and ease breathing.
- Home adjustments: Use HEPA air purifiers, safe bedding (e.g., paper or hemp), and maintain proper humidity (40%-60%).
- Nutrition: Provide high-quality protein, fresh vegetables, and supplements like Vitamin C or Omega-3s.
- Emergency readiness: Keep oxygen kits or rescue medications handy and monitor symptoms closely.
While these conditions are not curable, proper care can help your pet lead a comfortable life. Always consult your vet for tailored treatment plans and regular check-ups.
Respiratory Disease in Dogs and Cats – HORIBA Veterinary CPD Webinar
sbb-itb-e212914
Veterinary Care and Medical Treatment
Oxygen Therapy Methods and Costs for Pets with Respiratory Distress
Collaborating with a veterinarian to develop a customized treatment plan is critical for effectively managing chronic respiratory conditions in pets. Your vet will create a plan tailored to your pet’s diagnosis, symptom severity, and overall health. This approach ensures your pet can maintain their quality of life while addressing specific challenges, whether it’s feline asthma, chronic bronchitis, or tracheal collapse. By tackling these issues early, you can help prevent irreversible lung damage and other complications.
Medications Your Vet May Prescribe
Corticosteroids are often the backbone of treatment for respiratory conditions involving inflammation. These medications help reduce airway swelling and mucus production, making it easier for your pet to breathe. While oral prednisolone is frequently used initially, inhaled fluticasone is better suited for long-term management due to its lower risk of side effects. Interestingly, fluticasone binds to glucocorticoid receptors with about 20 times the affinity of dexamethasone, making it highly effective. In one study involving 246 cats with mild to moderate asthma, 81.7% (201 cats) transitioned off oral prednisolone within four weeks by switching to inhaled fluticasone.
Bronchodilators, such as albuterol, play a key role in relaxing the smooth muscles in the airways during breathing emergencies. While these medications provide fast relief, they are most effective when combined with corticosteroid therapy. For pets with chronic respiratory issues, antibiotics may also be necessary to address secondary bacterial infections. Nebulization is often used to deliver antibiotics, saline, or mucolytics directly to the lungs, which is particularly helpful when mucus is obstructing the airways.
To ensure medications work as intended, your vet may recommend overlapping oral and inhaled steroids for about two weeks. Inhaled medications should be administered using an aerosol chamber for optimal delivery.
If medications and nebulization don’t fully address your pet’s breathing issues, oxygen therapy may become necessary.
When Oxygen Therapy Is Needed
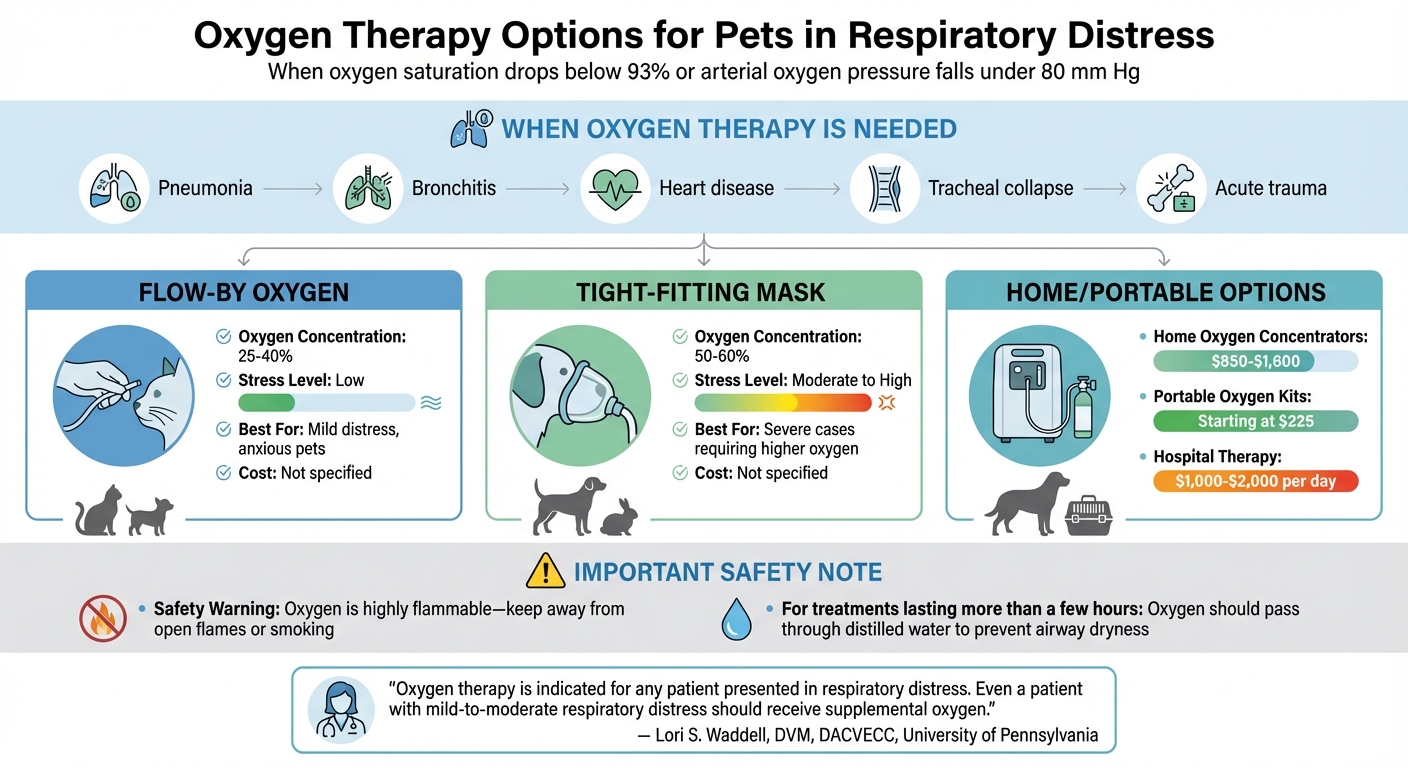
Oxygen therapy is essential when oxygen saturation drops below 93% or arterial oxygen pressure falls under 80 mm Hg. This treatment is particularly useful for conditions like pneumonia, bronchitis, heart disease, tracheal collapse, or acute trauma.
"Oxygen therapy is indicated for any patient presented in respiratory distress. Even a patient with mild-to-moderate respiratory distress should receive supplemental oxygen."
- Lori S. Waddell, DVM, DACVECC, University of Pennsylvania
The method of oxygen delivery depends on your pet’s condition and stress level. Flow-by oxygen, where a tube is held near the nose, can increase oxygen concentration to 25%–40%. For more severe cases, tight-fitting masks can deliver concentrations of 50%–60%. If your pet requires ongoing oxygen therapy, home oxygen concentrators are a cost-effective option, ranging from $850 to $1,600. Portable oxygen kits start at about $225, while hospital therapy can cost $1,000–$2,000 per day.
For treatments lasting more than a few hours, oxygen should pass through distilled water to prevent airway dryness. Always remember that oxygen is highly flammable – keep it away from open flames or smoking.
Regular Check-Ups and Monitoring
Ongoing veterinary care is crucial as your pet’s condition changes over time. Regular check-ups allow your vet to monitor progress, adjust medications, and catch potential complications early, such as pneumonia, weight loss, or fluid buildup. For bacterial respiratory infections, antibiotics often show results within seven days. However, if symptoms persist, your vet may need to modify the treatment plan. Chronic infections, like Mycoplasma in rats, may require "pulse therapy", which involves prolonged or intermittent antibiotic treatment cycles lasting 6–8 weeks.
Between visits, keep track of your pet’s respiratory rate, sounds, and hydration levels to help guide treatment adjustments. For example, you can check hydration by gently pulling up a fold of skin on your pet’s neck – if it returns slowly, this could indicate dehydration. Never give your pet human medications or drugs meant for other species, as improper dosages can lead to toxicity.
Adjusting Your Home Environment
Your home plays a big role in your pet’s respiratory well-being. While medical treatments are essential, simple tweaks to your living space can make a noticeable difference. Even the best medications may struggle to offset the effects of poor air quality or airborne irritants. For small mammals like hamsters, guinea pigs, and rabbits, their faster breathing rates make them especially vulnerable to changes in air quality. By focusing on reducing irritants and improving air conditions, you can help your pet breathe easier.
Eliminating Airborne Irritants
Start by identifying and removing common irritants that can harm your pet’s respiratory system. Smoke from tobacco or wood, VOCs from paints and new furniture, and air fresheners are some of the biggest culprits [23,24]. Cleaning products with bleach, ammonia, or chlorine, as well as aerosol sprays and scented candles, can also irritate sensitive airways [23,24]. Pet dander, which can linger in the air for a long time and even settle deep in the lungs, is another concern. In fact, dander can remain in your home for up to six months, even after the pet is no longer there [19,21].
Bird owners face an additional danger: fumes from overheated nonstick pans coated with Teflon can be deadly due to birds’ highly sensitive respiratory systems.
Using a HEPA air purifier can help significantly. These filters can trap up to 98% of allergen particles, improving air quality. Cleaning with damp cloths and HEPA-filtered vacuums further reduces airborne allergens [17,19,22]. Opening windows for a few minutes daily can also help clear out cooking fumes and chemicals, as long as outdoor pollen levels are low [19,23]. Be mindful that indoor air quality often worsens during winter when homes are sealed, trapping dust and fumes from fireplaces or candles.
Selecting Safe Bedding and Cage Materials
Once airborne irritants are under control, turn your attention to bedding and cage materials. These can have a direct impact on your pet’s respiratory health. Opt for dust-free paper bedding, hemp, or aspen shavings, which are safer for pets with respiratory sensitivities [25,26,28]. Avoid cedar shavings and non-kiln-dried pine, as they release harmful volatile aromatic hydrocarbons that can inflame airways and affect liver function.
"Never use cedar shavings as bedding as it can cause serious liver complications in pets."
- Pattie Larson, LVT
If your pet shows signs of respiratory distress, such as wheezing or sneezing, switch to dust-free paper or hemp bedding immediately [28,29]. Higher-quality paper bedding is a better choice than cheaper alternatives, as it minimizes respiratory risks. Fleece liners can also work well for pets that don’t chew on fabric, but they require frequent washing to manage odors [26,28].
Ventilation is another key factor. Cages with bars allow for better airflow, while glass aquariums or tanks can trap ammonia from urine, which can irritate your pet’s lungs. To prevent ammonia buildup, remove soiled bedding daily and perform a thorough cage cleaning weekly using mild, unscented soap [26,28].
Managing Humidity and Temperature Levels
Keeping humidity levels between 40% and 60% is essential for your pet’s respiratory health. Use a hygrometer to monitor humidity, and adjust it with a humidifier during dry seasons or a dehumidifier in damp conditions. Humidity below 40% can dry out nasal passages, making infections more likely, while levels above 60% can encourage mold, mildew, and dust mites – common respiratory triggers.
Place the hygrometer in the room where your pet spends most of its time for accurate readings. Small mammals like guinea pigs and rats are particularly sensitive to high humidity, which can worsen infections.
Temperature control is equally important. High temperatures can cause pets to pant excessively, adding unnecessary strain on their already sensitive respiratory systems. Use air conditioning or fans to maintain a cool environment, especially during hot weather, to keep your pet comfortable and stress-free.
Nutrition and Immune System Support
Good nutrition is a key player in helping your pet tackle respiratory challenges. Along with medical care and a healthy environment, the right diet can strengthen your pet’s ability to fight infections, reduce inflammation, and repair respiratory tissues. For pets with chronic respiratory conditions, what they eat is just as important as any other part of their care routine.
Meeting Your Pet’s Dietary Needs
Providing the right nutrients starts with high-quality protein, which is essential for tissue repair and maintaining a strong immune system. For small pets like rats and hamsters, lean options such as chicken or turkey can support recovery. On the other hand, herbivores like rabbits and guinea pigs thrive on constant access to grass hay, such as Timothy or Orchard grass. Skip alfalfa hay for adult herbivores – it’s too high in calcium and calories for their needs. Besides respiratory health, this type of hay also supports proper digestion, which is closely tied to overall immune strength.
When it comes to commercial food, avoid pellet mixes packed with sugar, fat, and fillers. For herbivores, pellets should make up no more than 5% of their diet. Fresh vegetables like leafy greens are a must; for example, dill has been shown to benefit guinea pigs. Birds, in particular, need variety – seed-only diets can cause severe vitamin A and calcium deficiencies, which often lead to respiratory infections and other health problems.
If your pet is congested and not eating well, try warming wet food for 10–15 seconds. This can boost the aroma and make the food more appealing, encouraging your pet to eat.
Using Supplements to Support Respiratory Health
Supplements can provide an extra layer of support for your pet’s respiratory system. Vitamin C is especially beneficial for guinea pigs and rats, as it strengthens the immune system and helps reduce inflammation in the airways. During recovery from respiratory infections, an extra boost of vitamin C can make a big difference. For birds, vitamin A is crucial – deficiencies in this vitamin, often caused by seed-only diets, are a common cause of respiratory issues.
Omega-3 fatty acids are another great option, as they reduce nasal inflammation and promote better respiratory function. Minerals like zinc and selenium are also important, helping to repair damaged tissues and prevent secondary infections. Probiotics, when given 1–2 hours after antibiotics, can protect your pet’s gut health and maintain immune balance.
If your pet stops eating due to illness, start syringe feeding immediately with a nutritional support formula like Nutri-Recovery to prevent serious complications. Staying hydrated is just as important – offer wet foods, low-sodium broths, or even tuna water to help thin mucus and make breathing easier.
Foods That May Worsen Respiratory Problems
Certain foods can be harmful to your pet’s respiratory health, so it’s important to know what to avoid. For example, avocado is toxic to rabbits and birds, causing respiratory distress and fluid buildup around the heart. Foods like onions, garlic, chives, and leeks can damage red blood cells, leading to anemia and rapid breathing as the body struggles to circulate oxygen. If you’re feeding baby food to a sick pet, always check the label – many contain onion or garlic powder.
Caffeine and chocolate are also dangerous, as they contain methylxanthines that can trigger rapid breathing, panting, and even respiratory failure. Alcohol and raw yeast dough, which produce ethanol, can cause severe respiratory depression. Even excess salt can raise body temperature and make breathing more difficult.
High-sugar foods should also be avoided. Obesity is a growing problem, with over 50% of pets in the U.S. being overweight. Extra weight doesn’t just strain the heart and lungs – it also causes low-grade inflammation that can worsen respiratory issues. Helping your pet lose weight through a controlled diet can greatly improve their breathing and overall health.
Conclusion
Managing chronic respiratory conditions in small pets involves a combination of regular veterinary care, thoughtful environmental changes, and proper nutrition. As discussed earlier, medications help control inflammation and ease airway constriction, while a toxin-free environment reduces potential triggers. At the same time, a well-balanced diet supports overall health and resilience.
While chronic conditions like bronchitis and asthma are not curable, they can be effectively managed to ensure a good quality of life. Dr. Melissa Boldan emphasizes, "With appropriate management, most cats with bronchitis can live long, full, high-quality lives". These principles apply to other small pets as well, highlighting the importance of the strategies outlined in this article.
Consistent vigilance plays a key role in managing these conditions. Small pets often hide signs of illness, and respiratory issues can escalate quickly. Watch for symptoms such as lethargy, unusual breathing sounds, the "orthopneic position" (standing with front legs spread and neck extended), blue or gray gums, open-mouth breathing, or persistent coughing. If you notice any of these signs, seek veterinary care immediately.
It’s also important to have rescue medications or oxygen kits on hand, as recommended by your veterinarian, to manage acute episodes. Additionally, recording videos of coughing or wheezing incidents can provide your veterinarian with critical information to fine-tune your pet’s treatment plan. This proactive approach strengthens the overall management strategy and supports your pet’s well-being.
FAQs
How can I tell if my pet’s breathing changes are an emergency?
Signs that your pet may be experiencing a breathing emergency include difficulty breathing, rapid or shallow breaths, open-mouth breathing, bluish gums, or increased effort and noise while breathing. If you observe any of these signs, it’s essential to get veterinary help immediately. Acting quickly could make all the difference in protecting your pet’s health.
What’s the safest way to give inhalers or nebulizer treatments at home?
To safely administer inhalers to pets at home, it’s important to use a spacer and mask specifically designed for animals. This helps ensure the medication is delivered effectively. Always stick to the dosage and technique recommended by your veterinarian.
If you’re using a nebulizer, opt for an ultrasonic device that produces particles in the 2-5 micron range, paired with a nebulization chamber or mask. Proper setup and medication use should always follow your vet’s instructions to achieve the best outcomes.
What air-quality and bedding changes help the most quickly?
Improving ventilation and opting for dust-free, hypoallergenic bedding can make a big difference in reducing respiratory irritation for small pets. By cutting down on dust and other irritants in their surroundings and ensuring proper airflow, you can significantly improve air quality and create a more comfortable environment for pets dealing with chronic respiratory issues.










